Varicose Veins – What You Need To Know | Palm Clinic
If you think you may have varicose veins, it’s important to understand the symptoms, causes, risks and management options that are available.
At Palm Clinic in Auckland, we have been treating varicose veins for over 25 years. Below we explain what you need to know about varicose veins and the recommended treatment options.
What Are Varicose Veins?
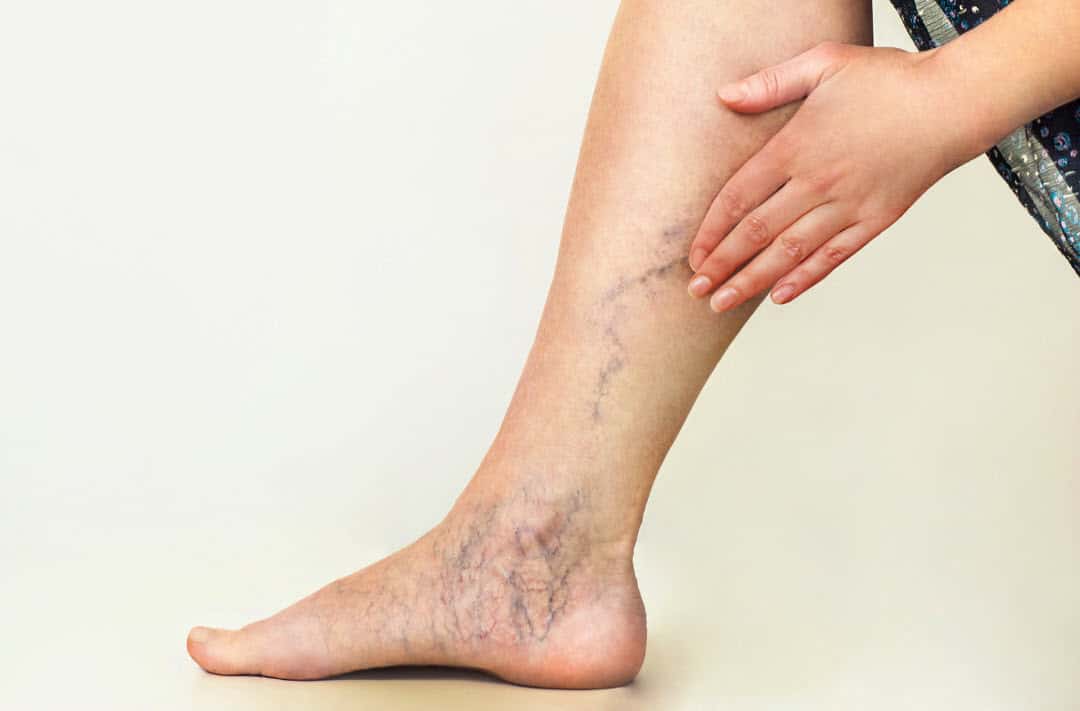
Varicose veins are enlarged swollen veins in the legs that often appear blue, green or dark purple. They are faulty veins that no longer pump blood through the leg as they should.
These photos show examples of how varicose veins may appear.
These photos show examples of how varicose veins may appear.


What Are The Symptoms Of Varicose Veins?
Varicose vein symptoms may include aching, pain or a feeling of heaviness or tiredness in the legs. People may also experience itchiness, cramps (especially at night) or restless legs.
Some people will have the visible symptoms of varicose veins but not the discomfort, while others may have the discomfort but no visible symptoms.
Discomfort is often relieved by elevating the legs or walking, and is exacerbated by standing or sitting still.
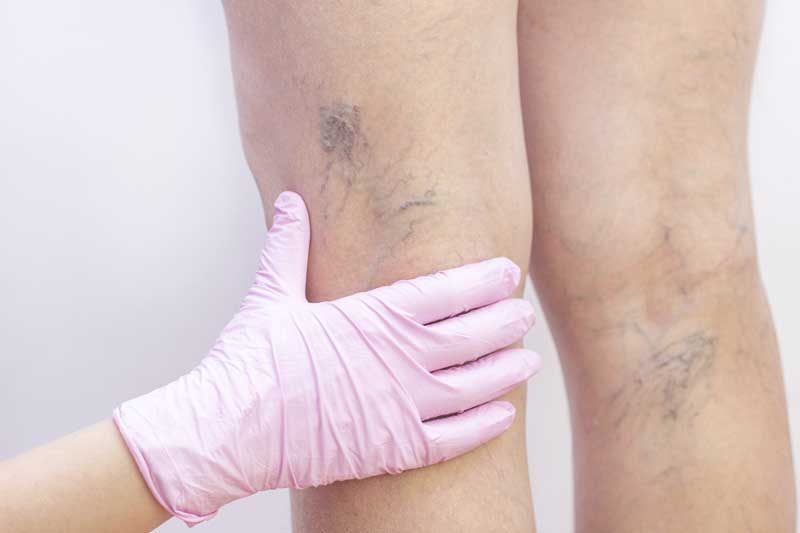
Having spider veins on the legs or feet is also a symptom of underlying varicose veins.
Photos of how spider veins may appear:
What Causes Varicose Veins?
Varicose vein causes are to do with ‘venous dysfunction’ also known as ‘venous insufficiency’. This is when the veins become weaker and are unable to pump blood through the legs.
Varicose veins are veins that have become stretched, inflamed and have lost their elasticity so that blood begins to pool within them causing them to swell.
Varicose veins causes include:
- Genetics as it is proven that you are more likely to develop varicose veins if you have a parent with varicose veins. Venous disease has a strong familial tendency. If one parent has varicose veins, you have a 50% chance of developing them. If both parents have varicose veins your chance of developing them is 90%.
- Being overweight as the additional weight puts additional pressure on the leg veins.
- Spending a lot of time on your feet, for example if your occupation requires long hours standing without moving around too much.
- Being female. Women are more likely to develop varicose veins as oestrogen weakens veins. Being female, taking the oral contraceptive pill or hormone replacement therapy, and pregnancies all add to the likelihood of developing venous dysfunction over time.
- Pregnancy as carrying extra weight puts extra pressure on the legs, as well as increased blood volume pumping through the veins. You can read more about varicose veins in pregnancy here.
- Ageing: Although varicose veins can be experienced by teens and young adults, they tend to become more prevalent with age.
How Common Are Varicose Veins?
Varicose Veins are very common with over 30% of the population having them in Western countries, or around 80% if you include reticular and spider veins. In those aged 40-80 they are twice as common in women than in men.
How Can You Manage Varicose Veins?
How To Manage Varicose Veins At Home
- Elevate the legs to allow the veins to drain during breaks and at the end of the day.
- Walk regularly to develop the calf muscle pump which helps the leg veins pump blood.
- Maintain a healthy weight to reduce excess pressure on the veins.
Wear compression stockings to improve vein efficiency and reduce the chance of deep vein thrombosis.
Varicose Vein Treatments
Surgical stripping was the treatment of choice in the past. This involved surgically removing all or part of the vein. It is no longer recommended as there are now less invasive methods which have fewer risks, less down-time and better long term results.
The gold standard treatment for varicose veins, as recommended by the National Institute for Health and Care Excellence, is Radiofrequency Ablation.
This treatment involves closing the varicose vein off from the inside, and once the vein is closed, the body absorbs it over a number of months. Recent studies continue to prove RFA is safe, effective and with few passing complications.
Any smaller veins can be treated with Ultrasound Guided Sclerotherapy.
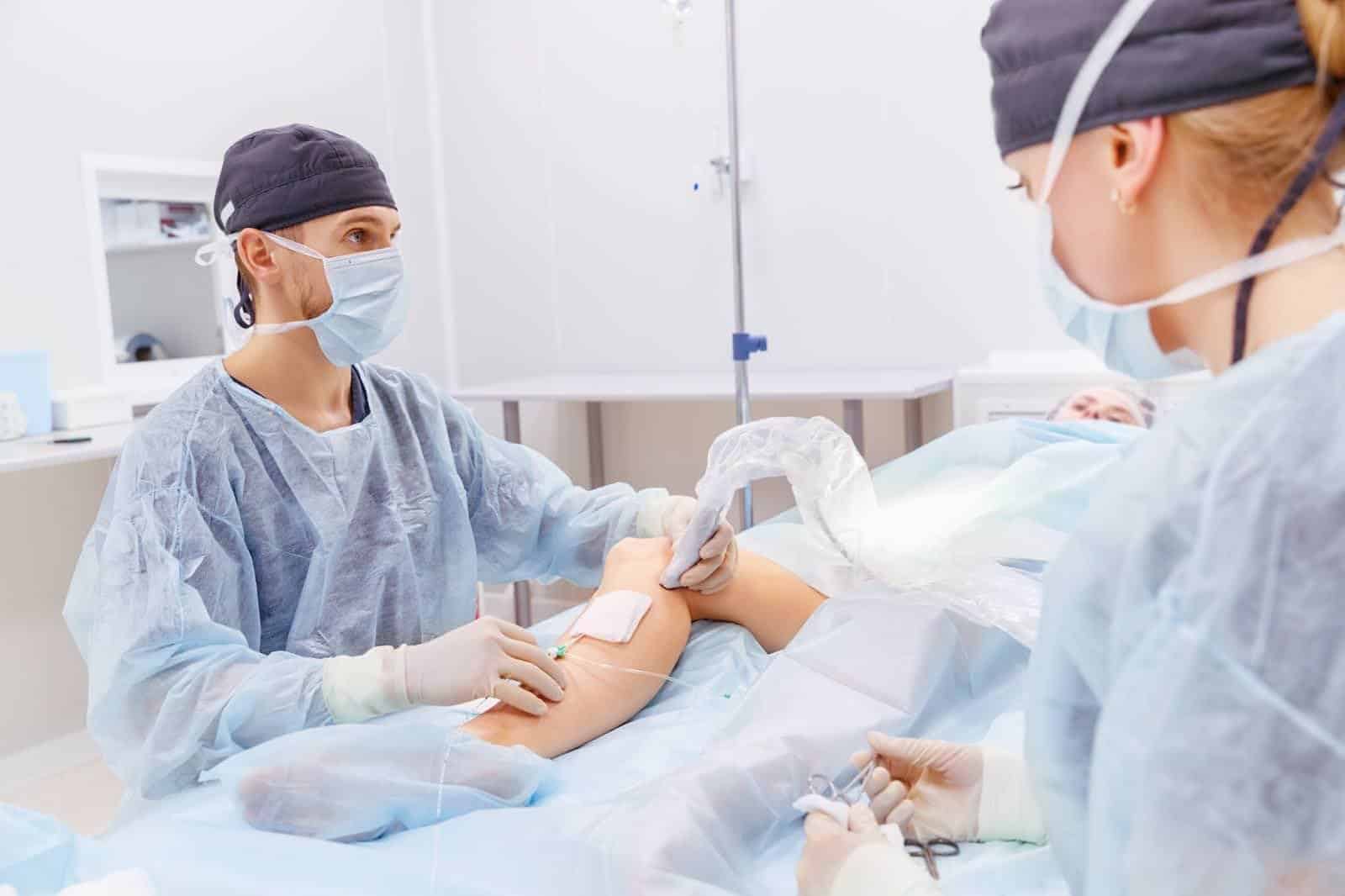
An example of Radiofrequency Ablation varicose vein treatment being performed:
What Happens If Varicose Veins Are Left Untreated?
In most cases, symptoms will worsen if veins are left untreated. The rate at which this happens can vary widely.
The presence of varicose veins increases the risk of experiencing deep vein thrombosis by five to six times.
The development of skin changes (pigmentation, eczema, ulcers) is usually a strong indication that it is time to proceed with treatment.
Read our blog post to learn more about the risks of leaving varicose veins untreated.
Explore Your Options At Palm Clinic
If you would like further advice or are considering varicose vein treatment, please contact our reception team to book in for a consultation. We have an experienced team of professionals at our skin and vein clinic who are here to help you navigate your options.